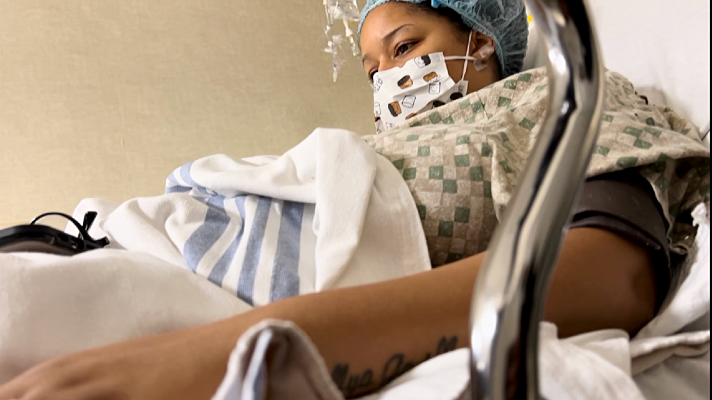
My uterus decided one day to go rogue, pulling off stunts that would make a professional acrobat blush.
It was like a rebellious teenager, causing discomfort and a whole lot of distress.
So, we (my uterus and I) needed an intervention and we dove headfirst into an episode of ‘Grey’s Anatomy’, complete with dramatic lighting and a heart-pounding soundtrack.
And so my decision to get pelvic organ prolapse surgery was a rollercoaster of emotions, medical jargon, and awkward conversations.
It came fully packaged with fear, uncertainty, and last-minute WebMD searches (0/10, would not recommend).
The plot twist?
That life-altering, slightly terrifying surgery turned out to be the best thing I’ve done.
No, seriously!
So, if you’re out there, wrestling with the same issues, flipping through the never-ending webpages of doom, looking for someone who gets it, this is for you.
Hold on to your uterus and pause your search for a beacon of understanding of internet self-diagnosis.
Allow me to share my story that admittedly teeters on the edge of TMI (spoiler alert).
I’ve been there, done that, and got the hospital socks to prove it.
This post is all about my pelvic organ prolapse surgery.
Table of Contents
Reader Beware: Let’s Get Things Straight!
Before we continue, I think it’s important to clarify a few things.
As you know, I am not a medical professional (I have a degree in English for Heaven’s sake).
This blog post, my website, and, frankly, anything you read on the internet should never be a substitute for professional medical advice, diagnosis, or treatment.
I’m sharing my journey in the hopes that it might help someone else navigate their own, but every situation is unique.
Every body is different.
What worked for me might not work for you, and that’s perfectly okay.
So if you’re experiencing symptoms or have questions or concerns about your health, please, please, please reach out to a healthcare provider.
Talk to a professional. They’re the experts, after all.
Remember, there’s no such thing as a stupid question when it comes to your health, and you should never feel embarrassed about seeking help.
You have every right to understand what’s happening with your body and to make informed decisions about your health.
What’s Up Down There?
So, let’s start with the basics.
What exactly is pelvic organ prolapse?
It’s a condition where the muscles and ligaments supporting your pelvic organs weaken, causing these organs to drop or press into the vagina.
It’s like when your underwear starts to sag because the elastic has lost its stretch, except this involves your internal organs (which is definitely way less fun).
Imagine the horror when I found out that my stage three prolapse meant that my uterus was hanging way too low, and my bladder (a cystocele) and rectum (a rectocele) were misbehaving, too.

Just How Far Down the Rabbit Hole Are You?
The stage of your prolapse is basically a measure of how far your pelvic organs have fallen.
It’s like a game of “how low can you go”, but with your organs instead of a limbo bar.
Stage 0 is the gold standard – all your organs are right where they should be.
Stage 1 is a mild prolapse, stage 2 is moderate, and by stage 3, one or more of your pelvic organs have really made a break for it.
At stage 4, or total prolapse, the affected organ is completely protruding from your body.
In my case, I was grappling with stage 3, the cheeky so-and-sos.
Rectocele and Cystocele: Meet The Uninvited Guests
Alright, let’s unpack these tongue twisters.
In the world of prolapse, rectocele and cystocele are two pesky sidekicks.
A rectocele happens when the rectum bulges into or out of the vagina, whereas a cystocele is when the bladder dips into the vagina.
To put it simply, it’s like your rectum or bladder is trying to stage dive into your vagina and let me tell you, it’s not a crowd-pleasing move.
I had both these interlopers, making my pelvic organ prolapse saga a true triple threat.

Weighing the Options: Surgery or Pessary – That’s the Question!
Now, if you landed here in your Google search of how to fix a prolapse without surgery, keep reading.
Pelvic organ prolapse doesn’t necessarily mean an express ticket to surgery town.
There were a few paths I could have taken to tame this unruly bunch.
You could go for physiotherapy or pelvic floor exercises to strengthen your muscles, lifestyle changes to reduce pressure on your pelvic organs (think maintaining a healthy weight and avoiding heavy lifting), or even hormone treatment.
One other notable contender is a pessary, a removable device placed into the vagina to provide support to the sagging areas.
Think of it like a really supportive bra but for your pelvic organs.
Honestly, I wasn’t entirely convinced of this option since I had a “falling out” experience with the NuvaRing (yes, you read that right).
However, it is an option worth considering, especially for those who aren’t ideal candidates for surgery or prefer a non-surgical approach.
Despite the options I had, I walked into my first appointment with my Urogynecologist knowing I wanted a hysterectomy, specifically a total hysterectomy.
Yup, I was retiring my uterus, and very happy to put it to rest after its hard work of three beautiful pregnancies and births.
Frustrated couldn’t even begin to describe the emotions I had at that time.
Thankfully, my husband was there as my advocate because I couldn’t form the words through my tears or disappointment and fear that was already stirring.
Important to note: make sure to check with your insurance to see which, if any or all, options will be covered.
My surgery, initially set for January, was postponed due to COVID-19, and then again on the day of my surgery, for an additional test.
Initially, under my husband’s insurance, we were preapproved for surgery, but he switched employers just before my [new] surgery date.
And under new insurance, I was hit with a major bill that wanted me to justify how my hysterectomy was any different than plastic surgery.
A Statistical Unexpected Plot Twist
Having recently written a post on Black Maternal Health, I feel it’s essential to mention it here too.
The glaring disparity in healthcare experiences between Black and white mothers is a harsh reality in our country.
Going into my first-ever surgery just months after losing my dad in the very same hospital – you can imagine the anxiety swirling in my mind.
It was like living in a horror movie, with the same hospital, the same white coats, and the fear of not waking up from the anesthesia.
Despite a couple of hiccups with my surgery date being postponed twice, my experience turned out to be nothing short of incredible.
My urogynecologist and the surgical staff were truly Godsent – providing me with the care, patience, and expertise I needed.
How long does it take to recover from pelvic organ prolapse surgery?
I was told it was supposed to be anywhere from three to eight months (sometimes longer, depending on the severity and the type of hysterectomy).
However, I was up and walking doing normal activities in 48 hours.
I am grateful for my experience but I understand that not every Black woman is as lucky.
The truth of the matter is, healthcare experiences are not always this positive for Black mothers, and that needs to change.
If you’re a mother, especially a Black mother, reading this, I want you to know you’re not alone.
Your fears are valid, but so are your hopes.
Keep asking questions, keep advocating for your health, and know that there are positive experiences out there.
My journey is a testament to that.
My Total Hysterectomy: The Full Monty (but Kept the Ovaries)
Since I’m not a medical professional, I’m not well versed in how many pelvic floor surgery types exist.
And despite being told by medical professionals in Florida that nothing could be done, the big day finally arrived in March.
Waking up from surgery, my first words were for my urogynecologist, not my husband.
Talk about a plot twist, right?
That’s how much I trusted my doctor.
Now, in my case, I had a total hysterectomy.
That’s doctor lingo for saying they took out my entire uterus – including the cervix, and fallopian tubes.
He actually went a step further by medically closing my now non-existent cervix and anchoring my pelvic wall to my back to prevent aging and gravity (aka a repeated prolapse).
Contrary to what you might think, a total hysterectomy doesn’t necessarily mean they take out everything.
I was able to keep both of my ovaries, thank you very much!
Why does that matter?
Well, ovaries aren’t just about making babies.
They’re the primary producers of hormones like estrogen and progesterone.
By keeping them, I was able to avoid symptoms of surgical menopause like hot flashes and hair loss.
So, nope, I didn’t suddenly transform into a human radiator, and my hair is just as glorious as it was pre-surgery.
And guess what?
No more periods!
No more cramps, bloating, mood swings, or any of the other monthly joys that come with menstruation.
Having dealt with very heavy periods since a young teenager, being iron-deficient, and having orthostatic hypotension, this was the best decision I could have ever made in my life.
Surgery was almost 18 months ago (as of writing this), and I cannot emphasize how amazing it feels to be able to stand, sit, and run without constantly feeling lightheaded.
Thank God!

Laparoscopic Hysterectomy: Less Is More
Alright, let’s get to the specifics, starting with a laparoscopic hysterectomy.
If you’ve ever been as confused as I was, don’t worry, it’s not a kind of dinosaur or a spell from Harry Potter.
It’s a minimally invasive surgery used to remove the uterus.
The term “laparoscopic” sounds fancy, but it’s just doctor-speak for using a laparoscope, a long, thin instrument with a high-resolution camera and a high-intensity light at the front.
During a laparoscopic hysterectomy, small incisions are made in your belly to insert the laparoscope and tiny surgical tools.
The surgeon then performs the operation while guided by images sent by the laparoscope to a video monitor.
Think of it as playing a high-stakes, incredibly important video game inside your body.

The DaVinci Surgery Robot: My High-Tech Surgical Sidekick
While I was going through my laparoscopic hysterectomy, I had a little extra assistance – from a robot.
Now, before you start picturing a Transformer-like machine wielding a scalpel, let me clarify.
The da Vinci System is a robot-assisted surgical device that allows surgeons to perform complex procedures with more precision, flexibility, and control than is typically possible with conventional techniques.
The robot’s arms enter the body through a series of small incisions, making it minimally invasive.
It’s not autonomous – think less Wall-E, more high-tech tool.
In other words, it’s fully under the control of the surgeon.
So you’re looking at less blood loss, lower risk of infection, and faster recovery time.
Remember how I said I was back on my feet in two days?
The da Vinci System was a big part of that.
In my case, the da Vinci robot-assisted surgery made my total hysterectomy more precise and helped me get back to my usual life quickly with minimal scarring.
So, even though the idea of a robot-assisted surgery might seem a bit sci-fi, I can attest to its real-world benefits!
The Two-Day Wonder and The Invisible Scar
Now, I’m not going to paint a rosy picture here – recovering from a total hysterectomy isn’t a walk in the park.
In my case, it involved being loopy on anesthesia (seriously, who asks for Blistex?), braving car rides home while managing orthostatic hypertension, and corralling three small children – all while feeling a tad green around the gills.
But only for 48 hours.
A huge perk of a laparoscopic hysterectomy is the recovery time.
Because it’s minimally invasive, you can expect a quicker recovery compared to traditional open surgery.
In my case, I was up and about in just two days!
I mean, I wasn’t exactly ready to run a marathon, but I could handle basic daily tasks like a champ (like keeping up with my three small kids).
If you’ve seen some of the horror stories on YouTube, you might think you’ll be left with a gigantic scar running down your stomach.
But because of the type of surgery I had done, I wasn’t cut open or left with a c-section-like scar.
I have four tiny scars on my belly and trust me, they’re hardly noticeable.
Well, except for my kids who always point them out.

Sex Post-Surgery: The Bedroom Reboot
Once the dust settled, I began to notice the difference.
No more periods.
No more hot flashes.
My energy levels were through the roof!
There was a little snag though – weight gain, particularly in the midsection.
Now, I’d always wanted to gain weight, but maybe not quite this much.
Struggling my whole life to gain weight, literally stuck at 110 lbs in my 00 jeans, I was 187 lbs post-surgery.
But hey, that’s a small price to pay, and it’s just given me a new challenge to tackle in the gym.
Now, let’s talk about the elephant in the room: sex after a hysterectomy.
I won’t lie, things were different (remember my cervix was removed and closed, making my Beverly shorter).
But different doesn’t mean bad – it just means change.
Communication became even more important, as did trying new things.
As I healed, it kind of felt like going back to those exciting early days when you discovered the meaning of “hot and bothered.”
It was like rediscovering each other all over again, and in some ways, it made our bond even stronger.
This post was all about my pelvic organ prolapse surgery.
My vaginal prolapse surgery story – one woman’s journey from “Why me?” to “Well, that wasn’t so bad, now, was it?”
Even with a few bumps in the road, the destination was totally worth the trip.
I hope my experience from an actual patient perspective side can shed a little light, and remind you that no matter what, you’re stronger than you think.
If you’re hankering for more behind-the-scenes glimpses into my life, head on over to Instagram.
My feed’s a mixed bag of candid reflections, daily adventures, and the occasional pictures of my fur kids – because who doesn’t love those?
And if this post had you nodding along, then take a peek at these:
- How Pelvic Organ Prolapse Symptoms Are Ruining My Mom Life
- Surviving Black Maternal Health: How I Had 3 Amazing Births
- 9 Products To Get Rid of Postpartum Smell
No matter where you are on your journey, always remember this: you’re never alone, and you’re perfect just as you are.
Yes, society might be hounding us to “bounce back,” but here’s a thought – maybe bouncing back isn’t all it’s cracked up to be.
Instead, why not appreciate the hand pats on our “jiggles” from those tiny fingers?
Each one is a sweet reminder of our incredible bodies that stretched (literally) to the limits to create the little humans who adore us, jiggles and all.