If you’re not sure if you have pelvic organ prolapse symptoms, consider yourself lucky. But if you clicked the post, then I assume you’re also experiencing pelvic organ prolapse symptoms. Don’t worry, we’ll break it down in this post to give educational background as to how it ended up ruining my mom life.
This post is all about pelvic organ prolapse symptoms.
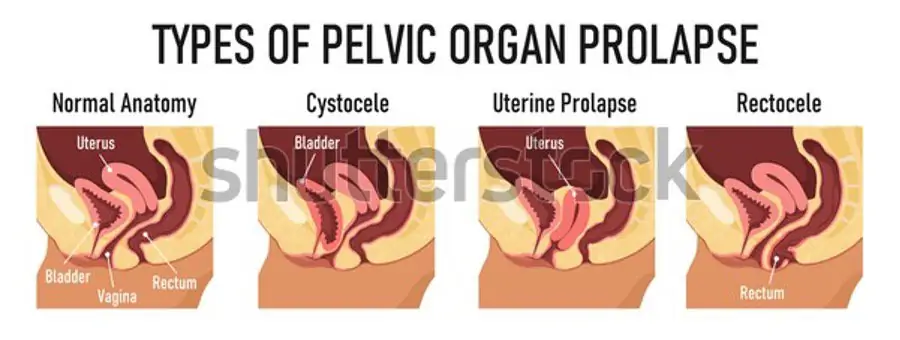
Pelvic organ prolapse is a condition of gynecology in which the pelvic organs herniate or descend in the vagina due to muscular or ligament weakness during pregnancy.
Statistics reveal that around 200,000 surgeries of POP are being performed annually in United States1. The incidence of Pelvic Organ Prolapse is increasing and is expected to reach 4.9 Million, a 46% rise by 20502.
What Causes Pelvic Organ Prolapse?
The main reason for Pelvic Organ Prolapse is the weakness or rupture of tissues or ligaments holding the pelvic organs like the bladder, uterus, vaginal wall, and rectum. There are some predisposing factors to the prolapse; these include:
- Vaginal Childbirth: Vaginal Parity may increase the risk of Pelvic Organ Prolapse; as the chances improve with several childbirths. However, it can occur even if you don’t have any children or Cesarian section4 5.
- Pressure on your abdomen: From obesity, coughing, or constipation.
- Having an overweight baby (above 8-9 pounds)6.
- Aging: With the advancement in age, chances of pelvic organ prolapse increases7.
- Hormonal changes during menopause also affect the onset of Prolapse8.
- Genetics also plays a role in Pelvic Organ Prolapse9.
Stages of Pelvic Organ Prolapse:
There are four stages of the pelvic organ prolapse, which depend upon the type of organ (uterus, bladder, rectum, vaginal wall) and the severity of the prolapse.
First-Degree prolapse: Organs slip down but only slightly.
Second-Degree prolapse: Organs slip down till the opening of the vagina.
Third-Degree prolapse: Womb or Vagina may bulge around 1 cm through the vaginal opening.
Fourth-Degree prolapse: This is a severe prolapse, and organs may protrude more than 1 cm.
Pelvic Organ Prolapse Symptoms:
Mild cases don’t have obvious signs. However, severe cases depict the following signs810:
- Feeling of pushing down something.
- a feeling of having a foreign object in your abdomen with aching, fullness, and discomfort.
- Difficult and leaking urination frequently (weakened bladder).
- Abdominal pain during intercourse.
- Difficult bowel movement.
- Vaginal bleeding and pressure sores.
Correction and Treatment of Pelvic Organ Prolapse:
Asymptomatic patients usually don’t require any treatment. However, correction and treatment of pelvic organ prolapse are needed when symptoms of abdominal pain, discomfort, sexual dysfunction, abnormal urination, and bowel movement are experienced. The conservative approach is helpful for women who can’t bear or undergo surgical interventions. The following correction procedures can be performed depending upon the choice of patients.
- Vaginal Pessaries:
It is a device placed inside the vagina to help relieve pelvic organ prolapse by easing the bowel movement and supporting the pelvic organs. Vaginal pessaries should be set correctly to avoid issues during daily workouts and chores.
- Pelvic Muscle Exercises:
Exercises that strengthen the pelvic muscles help relieve the symptoms of prolapse11.
- Hormonal Therapy:
Topical and systemic estrogen hormone therapies are beneficial in correcting the muscle tone of pelvic organs12.
- Surgical Intervention:
It is the last resort if the conservative approach doesn’t work and prolapse is severe. A variety of surgical procedures are available.
Primarily reconstructive surgery is performed. As an alternative, the Obliterative method can be applied to patients who can’t go for extensive surgery13.
If you thought this was helpful, please subscribe to my YouTube channel to watch my personal journey with prolapse here. Otherwise, stay tuned for my surgical updates right here on Do You Even Mom.
REFRENCES:
- Thompson CD, Henderson BE, Stanley R. Bladder calculi causing irreducible urogenital prolapse. BMJ Case Rep. 2018;2018. doi:10.1136/BCR-2018-225695
- Wu JM, Hundley AF, Fulton RG, Myers ER. Forecasting the prevalence of pelvic floor disorders in U.S. Women: 2010 to 2050. Obstet Gynecol. 2009;114(6):1278-1283. doi:10.1097/AOG.0B013E3181C2CE96
- Types Pelvic Organ Prolapse Cystocele Uterine Stock Vector (Royalty Free) 1742221451. Accessed December 25, 2021. https://www.shutterstock.com/image-vector/types-pelvic-organ-prolapse-cystocele-uterine-1742221451
- Dietz HP, Gómez M, Atan IK, Ferreira CSW. Association between vaginal parity and rectocele. Int Urogynecol J. 2018;29(10):1479-1483. doi:10.1007/S00192-017-3552-8
- Yan W, Li X, Sun S, et al. [Risk factors for female pelvic organ prolapse and urinary incontinence]. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2018;43(12):1345-1350. doi:10.11817/J.ISSN.1672-7347.2018.12.010
- Fonti Y, Giordano R, Cacciatore A, Romano M, Rosa B La. Post partum pelvic floor changes. J Prenat Med. 2009;3(4):57. Accessed December 25, 2021. /pmc/articles/PMC3279110/
- Chow D, Rodríguez L V. Epidemiology and prevalence of pelvic organ prolapse. Curr Opin Urol. 2013;23(4):293-298. doi:10.1097/MOU.0B013E3283619ED0
- Pelvic organ prolapse | Office on Women’s Health. Accessed December 25, 2021. https://www.womenshealth.gov/a-z-topics/pelvic-organ-prolapse#references
- Urogynecologic Surgical Mesh Implants | FDA. Accessed December 25, 2021. https://www.fda.gov/medical-devices/implants-and-prosthetics/urogynecologic-surgical-mesh-implants
- Pelvic organ prolapse: Overview. Published online August 23, 2018. Accessed December 25, 2021. https://www.ncbi.nlm.nih.gov/books/NBK525783/
- Li C, Gong Y, Wang B. The efficacy of pelvic floor muscle training for pelvic organ prolapse: a systematic review and meta-analysis. Int Urogynecol J. 2016;27(7):981-992. doi:10.1007/S00192-015-2846-Y
- Tzur T, Yohai D, Weintraub AY. The role of local estrogen therapy in the management of pelvic floor disorders. Climacteric. 2016;19(2):162-171. doi:10.3109/13697137.2015.1132199
- Chung S-H, Kim W Bin. Various Approaches and Treatments for Pelvic Organ Prolapse in Women. J Menopausal Med. 2018;24(3):155. doi:10.6118/JMM.2018.24.3.155

2 comments
It’s scary to think we aren’t told enough about these things during pregnancy!
They forget to mention A LOT in health class smh.